Useful Articles by Esthesion
On our blog, you will find practical tips, interesting facts from the world of dentistry, and answers to questions that may come to mind when caring for your teeth. We write clearly, openly, and with respect for your health.
Peri-Implantitis — When Inflammation Threatens Your Implant
Is the gum around your implant bleeding? Is it red or slightly swollen? Have you...

Dental Implant Care — How to Extend Their Lifespan to 20+ Years
A dental implant is an investment in the range of tens of thousands of Czech...

Full Mouth Reconstruction: A Complete Guide from Dentures to Implants
Every fourth patient who comes to us asking about full mouth reconstruction says the same...
Prevention Is Key: Why You Should Not Underestimate Regular Dental Check-Ups
Maybe nothing hurts, maybe you feel everything is fine. But that is exactly why it...

Why Regular Dental Hygiene Is More Important Than You Think
Most people associate a visit to the dentist with pain or with fixing problems that...
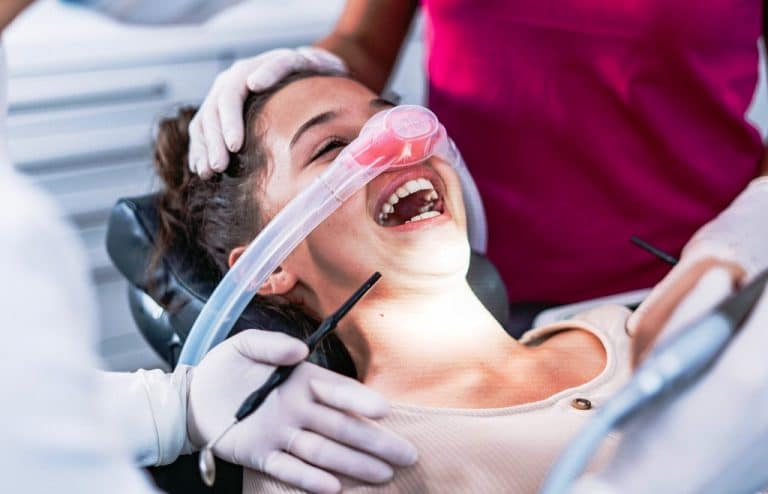
Laughing Gas (Analgesic Sedation): A Calm and Pain-Free Dental Visit
Fear of the dentist is a common reason why many people postpone necessary treatment. At...
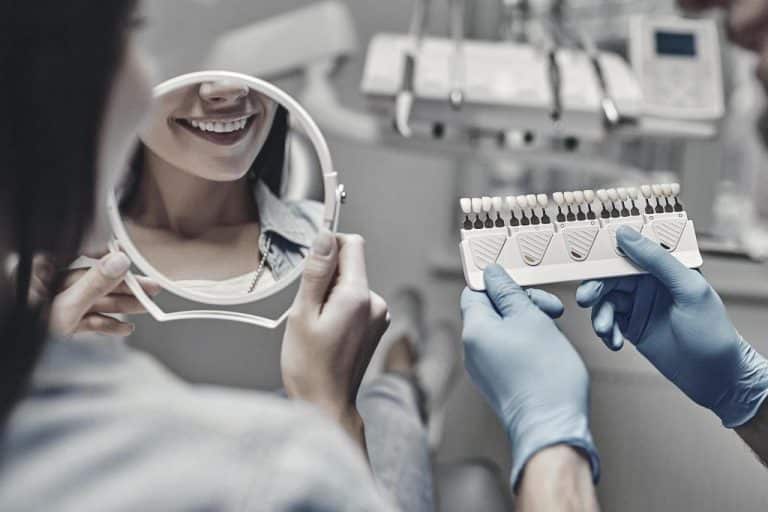
Dental Veneers: Everything You Need to Know on the Way to a Perfect Smile
Do you dream of a smile that truly makes you shine? Veneers are a modern...
Teeth Whitening: The Path to a Radiant Smile
Do you dream of a beautifully white smile? Teeth whitening is one of the most...

Peri-Implantitis: The Silent Enemy of Dental Implants
Peri-implantitis is a chronic inflammation of the soft and hard tissues surrounding a dental implant....
